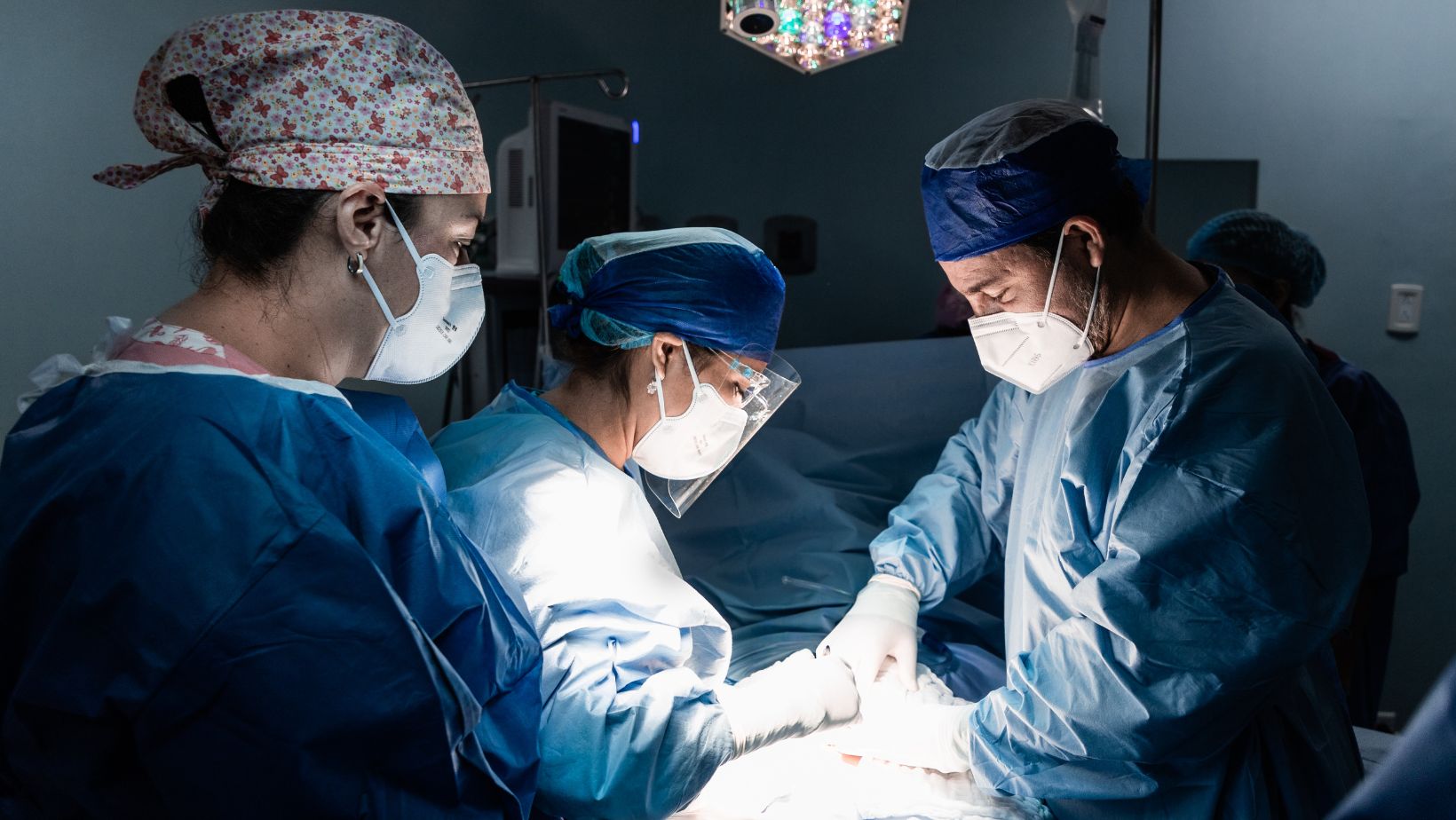
Because the Depth of an Open Abdominal Wound
In my years of medical writing, I’ve found that understanding the nuances of wound care is crucial, especially when it comes to open abdominal wounds. These wounds, often a result of surgery or trauma, can be complex and require a keen eye for detail, particularly in assessing the wound’s depth.
Diagnosing and Assessing Open Abdominal Wounds
The process of Diagnosing and assessing open abdominal wounds is pivotal in predicting wound healing outcomes and potential complications. There are multiple methods employed by professionals, each offering a certain degree of reliability.
It’s worth noting that no technique is faultless. However, a combination of these methods can offer the most accurate results. Let’s delve into the common diagnostic approaches.
Physical Examination
Physical examination holds a key part in the evaluation of open abdominal wounds. It’s typically the first step as it provides immediate, cheap, and critical information. Through examination, I inspect the wound for signs of infection like redness, swelling, and pus. I also try to approximate its depth, as even a cursory estimation can offer substantial information about the wound’s severity.
Additionally, it helps me assess vital signs such as the patient’s pulse, blood pressure, and temperature. Though it’s not 100% accurate, physical examination provides a cornerstone in the diagnostic process. It directs the path for future, more detailed, assessments.
Imaging Tests
Imaging tests are the second line of defense in the diagnostic process. Common imaging techniques include X-rays, Ultrasounds, CT scans, and MRIs. Each method has its unique advantages and can reveal different aspects about an open abdominal wound.
For instance, an X-ray can highlight an incisional hernia, while a CT scan is great for identifying abscesses or hematoma formations.
Diagnostic Peritoneal Lavage
Diagnostic Peritoneal Lavage (DPL) is another method that’s usually reserved for more severe open abdominal wounds. It’s an invasive technique in which a catheter is inserted into the abdomen. The aim is to confirm or deny the presence of internal bleeding, bacteria, or other possible complications within the abdominal cavity.
DPL has a high accuracy rate, in both assessing the depth of the open wound and detecting additional pathologies. However, due to its invasive nature and costs, it isn’t employed as a first-line diagnostic modality.
In winding up, remember that accurate wound assessment is imperative to delivering the most effective wound care. Particularly with open abdominal wounds, the depth of the wound significantly impacts treatment and recovery. The physical examination, imaging tests, and Diagnostic Peritoneal Lavage are all essential components in constructing an informed and effective treatment approach.
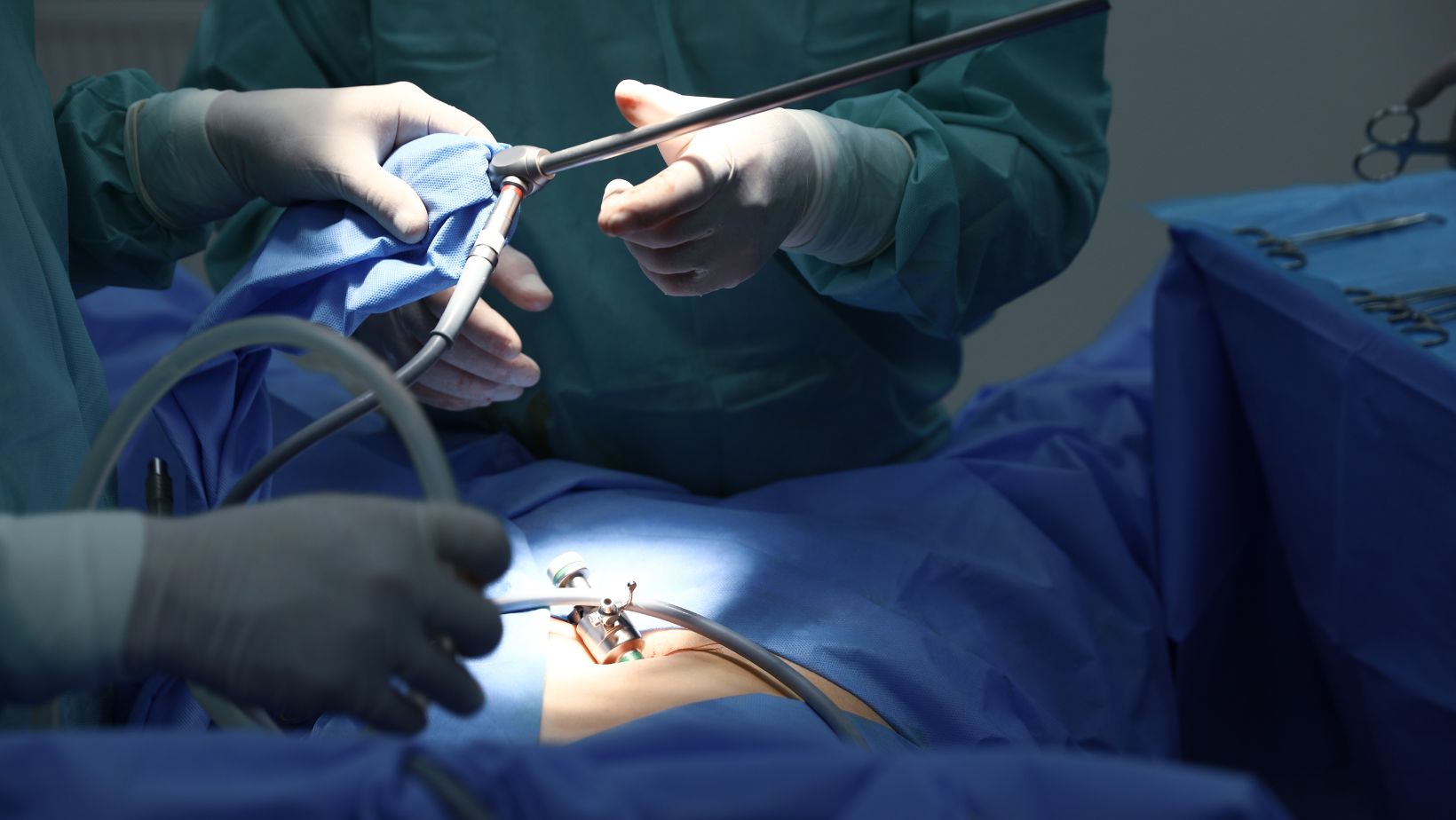
Treating Open Abdominal Wounds
After assessing the depth of the wound, it’s essential to move on to the next critical step in wound care—treatment. Keep in mind that the treatment of open abdominal wounds often varies depending on the patient and the severeness of the wound.
Stabilizing the Patient
Stabilizing the patient is the initial step in the process. A stable, calm patient often leads to better treatment outcomes. This process involves:
- Monitoring vital signs: Blood pressure, pulse, and respiratory rate are critical indicators of the patient’s overall condition.
- Administering pain management: Pain can exacerbate patient stress and impede the healing process, so addressing this quickly is vital.
- Ensuring patient comfort: Positioning the patient comfortably can ease tension and facilitate a smoother treatment process.
Cleaning and Debriding the Wound
Once the patient is stable, the focus shifts to the wound itself. The primary goal in this stage is to clean and debride the wound to prevent infection and promote healing:
- Cleaning the wound: Here, we gently rinse the wound with a saline solution to remove any foreign substances.
- Debriding the wound: Dead tissue can interfere with wound healing. Depending on the case, I might use surgical, mechanical, or enzymatic debridement.
Closing the Wound
The last step usually involves closing the wound. This can either be done immediately (primary closure) or after some days (secondary closure). It’s also worth noting that not all wounds must be closed; for some, especially infected ones, it’s better to leave them open under controlled conditions.
- Primary closure: If the wound is clean and there’s no risk of infection, stitching it closed immediately is the best route.
- Secondary closure: If the wound is dirty or infected, we may choose to clean it, leave it open, and only close it after several days.
- Tertiary closure: In some severe cases, wound packing might be done for several days before closing it.
By effectively following these steps, we can ensure proper healing and minimize complications. This process is certainly not a straightforward one, and it’s essential for professionals to make decisions based on a thorough understanding of the patient’s unique circumstances.